Since COVID-19 first appeared in 2020, the public has often tried to compare it with the flu. When you’re fighting an invisible enemy, finding similarities with something we are trained to recognize can be reassuring.
But how alike are COVID-19 and other common respiratory and sinus-related diseases, really? We took a closer look, comparing and contrasting a few diseases with information available through the Centers for Disease Control and Prevention. Here’s what we know.
Symptoms
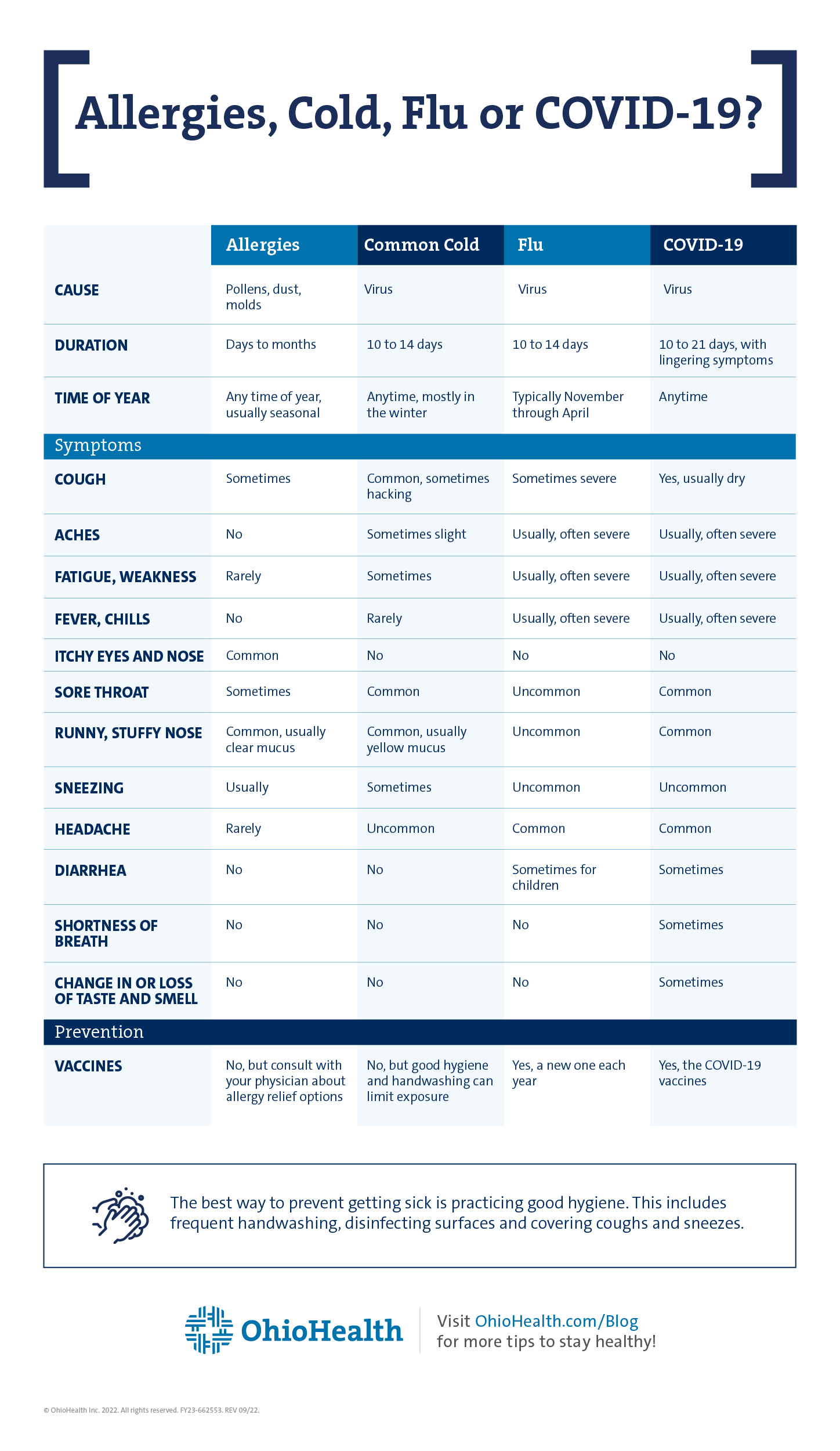
Similarities: Symptoms range from no symptoms (asymptomatic) to severe symptoms. Common symptoms for COVID-19 and the flu include fever or feverish/chills, cough, shortness of breath or difficulty breathing, sore throat, fatigue, runny or stuffy nose, muscle pain or body aches, headaches, vomiting and diarrhea. The common cold sometimes includes fatigue, fevers, and aches. Generally, allergies lead to symptoms of sneezing, itchy eyes/nose, and runny or stuffy nose.
Differences: Allergy symptoms can appear at any time and can last from days to months, depending on the cause. Flu and common cold symptoms appear more quickly, usually within one to four days. COVID-19 symptoms may not appear for two to 14 days after exposure to the virus. A unique symptom of COVID-19 is change in or loss of taste or smell.
Vaccinations have shown to greatly reduce symptoms in breakthrough cases of COVID-19. It is important to note that new symptoms are arising, and not all symptoms are always present, according to the Ohio Department of Health. If you feel sick, stay home and call your doctor.
Risk
Similarities: Everyone is susceptible to any of the conditions and viruses. Older adults, those with other health conditions and pregnant people are at a higher risk of developing severe symptoms and are at an increased risk for COVID-19 and influenza.
Differences: School-aged children infected with COVID-19 are at higher risk of Multisystem Inflammatory Syndrome in Children (MIS-C), which is a rare but severe COVID-19 complication.
Complications
Similarities: Common complications for COVID-19 and the flu include pneumonia, respiratory failure, acute respiratory distress syndrome, sepsis, cardiac injury, multiple organ failure, worsening of chronic medical conditions, inflammation of the heart, brain or muscle tissues, and secondary bacterial infections. With the common cold, complications can include ear pain/infection, fever, and asthma flare-ups.
Differences: COVID-19 has also been associated with blood clots in the veins and arteries of the lungs, heart, legs or brain, as well as Multisystem Inflammatory Syndrome in Children (MIS-C).
Transmission
Similarities: Transmission of COVID-19, the flu and the common cold seems to be almost identical. Both diseases are spread easily from person to person through small respiratory droplets containing the virus. These droplets appear when someone coughs, sneezes or even talks. It’s also possible that a person can contract the virus by touching surfaces where these droplets land and then touching their eyes, nose or mouth.
You can spread any of the three to others without being aware you are infected. It’s important to follow recommendations to stop the spread, like mask-wearing, social distancing and hand hygiene.
For the common cold, the flu and COVID-19, practicing good hygiene can help prevent the spread.
Differences: While it seems COVID-19 and the flu spread similarly, COVID-19 is more contagious amongst certain age groups and populations. COVID-19 can spread quickly and easily to many people, resulting in a higher continuous spread than the flu. The COVID-19 infectious period is about 2 days prior to symptoms and up to 10 days after symptoms appear, while someone with the flu is contagious from one day prior to symptoms appearing up until 7 days after symptoms appear. Infants and those who are immunocompromised can be contagious for longer periods of time.
Allergies cannot spread from person to person. There may be common triggers for people, like pollen or ragweed, but symptoms and experiences depend on the individual.
Prevention
Similarities: The actions we take to prevent the flu and common cold work against COVID-19 as well. These include frequent hand hygiene, mask-wearing, social distancing, disinfecting surfaces, and covering coughs and sneezes with a tissue or sleeve.
Differences: A new flu vaccine is released each year to help prevent infection. The CDC also recommends that everyone 6 months and older get a 2024–2025 COVID-19 vaccine.
Testing
Similarities: We can test for the flu and COVID-19 to confirm infections.
The CDC advises the following people should get tested for COVID-19:
- People who have symptoms of COVID-19.
- People who have come into close contact with someone with COVID-19:
- Those up to date on their COVID vaccinations should be tested 5–7 days after their last exposure.
Differences: There are no specific tests to detect a common cold or allergies. Comparing and contrasting symptoms or eliminating the possibility of other possibilities, such as influenza or COVID-19, can help determine a diagnosis of cold or allergies.
Treatment
Similarities: Some over-the-counter medications, such as acetaminophen, can be used to manage symptoms of any of the conditions discussed above. Antibiotics should not be used to prevent or treat the flu, COVID-19 or other viruses, like the common cold.
Differences: There are antiviral medications that can shorten the duration of the flu, ease symptoms and prevent complications.
Regardless of a patient’s vaccination status, COVID treatments are available for at risk individuals with mild to moderate COVID. The FDA has authorized or approved several antiviral medications used to treat mild to moderate COVID-19 in people who are more likely to get very sick.
For seasonal allergies, consider an allergy medication, such as Zyrtec or Claritin D, to help manage symptoms. For further information on managing specific allergy symptoms, contact your primary care provider.
Infection and mortality rates
Similarities: The common cold and allergies are significantly more common than COVID-19 or the flu, but the mortality rates for those conditions are essentially nonexistent. While some COVID-19 and flu cases do result in death, the majority of cases are mild.
Differences: Each year in the United States, the average adult will have 2-3 colds, while children usually experience more. For allergies, approximately eight percent of Americans experience it each year.
COVID-19 mortality rates have changed tremendously since the rollout of vaccines. People who contract COVID and are vaccinated are significantly less likely to die.
If you find yourself questioning what you are feeling, listen to an episode of The Wellness Conversation about navigating life post-pandemic here.
The information in this article was updated in September 2024.