COVID-19, flu or a cold? Many people are stuck on this question right now. So we sat down with OhioHealth’s system medical director of Infectious Diseases Joseph Gastaldo, MD, during a recent Facebook Live event to clear up the confusion.
We’ve included time stamps in our story to help you listen along to Dr. Gastaldo’s answers in the video above. As you read on, keep in mind that this information shouldn’t replace the advice of your doctor. If you have additional questions, visit the Centers for Disease Control and Prevention COVID-19 website.
What are the differences between flu and COVID-19? (01:17)
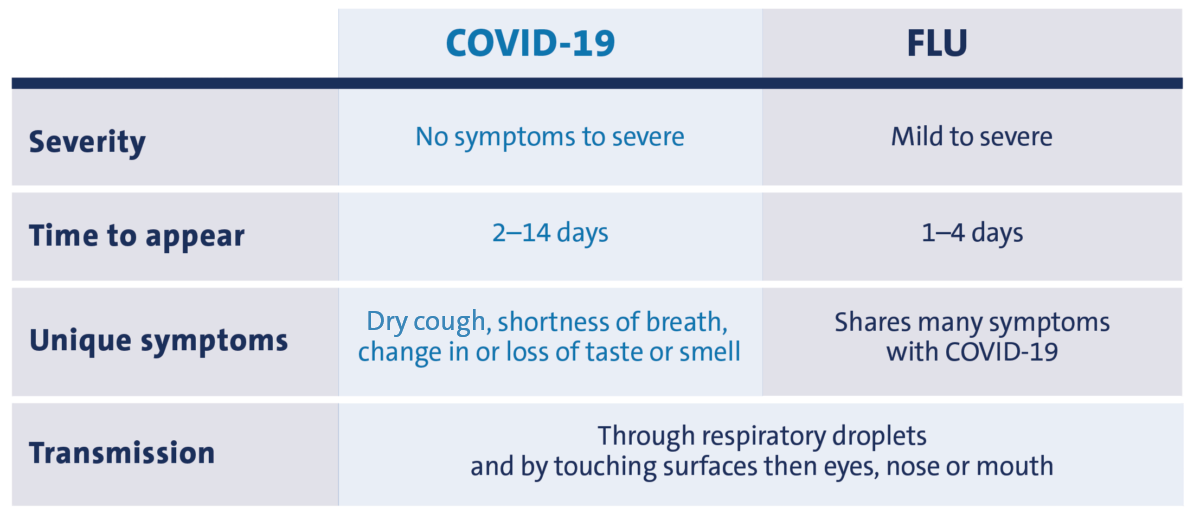
Influenza, or flu, and SARS-CoV-2, or COVID-19, while very similar, are not the same kind of virus.
Both viruses share all except two symptoms: a drier cough, and a loss of taste or smell. These two symptoms are unique to COVID-19. With COVID-19, symptoms can take five to 14 days to appear, while symptoms for flu appear within one to four days.
The same people are at risk for both viruses, except when it comes to children. Children have a higher risk of severe illness with flu than with COVID-19. On the contrary, children are rarely at risk with COVID-19.
Transmission is essentially the same for COVID-19 and flu. Primarily, these viruses are spread through droplets. However, there is a theory that COVID-19 is airborne.
Once we hit flu season, it’s very important that your healthcare provider considers both illnesses if you are showing symptoms. I recommend visiting the CDC website and familiarizing yourself with the described symptoms of influenza and COVID-19, which are updated promptly as new information comes to light.
Why is it more important that I get the flu vaccine this year? (04:44)
If you have COVID-19 symptoms and you’ve gotten the flu vaccine, your clinician will know that your symptoms are more likely due to COVID-19 and not flu. This is very important because it means treatment can be started sooner.
Every year, influenza is a major cause of death and hospitalizations. This year, we don’t know what’s going to happen in the winter. People are going to be inside more, and there will be lower humidity in the air. Both of these situations are friendly to COVID-19, increasing the risk of more people getting sick. On top of all of this is the fear of influenza as well, so it’s best to protect yourself in any way you can.
Is it safe to get the flu vaccine? (06:20)
Absolutely. It’s a huge myth that you can get influenza from the influenza injection or vaccination. This is physiologically impossible. There are a couple reasons as to why people may get sick after receiving the flu vaccine.
First of all, the flu vaccine does not give you protection from all of the influenza viruses that are out there. Every year, the CDC and the World Health Organization (WHO) make their best scientific guess as to what the predominant strains will be during flu season. The current vaccine can only give you antibody protection for four types of influenza. Sometimes the CDC and WHO get it right, but they can get it wrong. This is what we call a mismatch between the predominant strain.
Secondly, not everybody develops an immune response to the influenza vaccine. As you get older, you don’t take vaccines as well, which can affect the antibody protection you receive. Also, certain medications can interfere with the effectiveness of vaccines.
Unfortunately, the influenza vaccine is imperfect. However, it’s still something that saves lives every year.
Will there be a larger supply of the flu vaccine this year? (08:10)
Yes. The companies that make the influenza vaccination have increased their manufacturing capacity by about 15%.
When is a good time for me to get the flu vaccine? (08:40)
Getting the flu vaccine this year may be a little more challenging than it has in the past. It’s common for people to get the flu vaccine from the place they work. Considering a lot of people are working virtually right now, they may not have access to that service. There’s also challenges now with getting into the doctor’s office due to COVID-19 restrictions. Because of these new challenges, I would recommend getting the flu vaccine when it’s easy and convenient for you. If you find that you have an opportunity to receive the vaccine, I would advise getting it done to avoid any challenges presenting themselves later on.
Can I get COVID-19 and flu at the same time? (09:56)
The simple answer to that is yes. It’s my clinical hunch that if you were diagnosed with both viruses, you’re going to be sicker and potentially may need to be hospitalized. That being said, there are still a lot of unknowns. If you get COVID-19, are you at a higher risk to get influenza? If you get influenza, are you at a higher risk to get COVID-19? We just don’t know that yet.
Can I be tested for both flu and COVID-19 at the same time? (10:26)
Yes, and OhioHealth is working on a combined test we plan to have available sometime in October. It will comprise of one swab that will be used to test for both influenza and COVID-19.
In the future, could the flu vaccine be combined with a COVID-19 vaccine? (10:55)
If I had to guess now, I would say we’ll have a COVID-19 vaccine sometime in 2021 that will be on a cycle where you get it every year or every other year. Historically, vaccinations are combined. A classic example is hepatitis A and hepatitis B. When these vaccines first came out, they were separate. However, later on they were combined. So, if it’s proven that we need to get both vaccines on a regular basis, I’m optimistic we’ll have a COVID-19 and flu vaccine in the future.
Why do respiratory viruses spike in the winter? (11:51)
It’s multifactorial, but the gist of it is because we’re all inside. With respiratory viruses, outside is always better than inside because you have dilution of air and, therefore, good airflow. Inside is more challenging because the airflow, in a lot of cases, isn’t the best. So, more people in confined spaces, with a lack of airflow and a decrease in humidity, creates a friendly space for respiratory viruses to grow and spread.
If I start developing symptoms of flu or COVID-19, what are the first steps I should take? (12:58)
The first step is to ask yourself how you’re feeling. If you’re having difficulty breathing or you’re passing out, you need to call 911 immediately. If you’re stable and you’re doing well, you need to reach out to a primary care physician or provider. I know a lot of providers are doing very neat things with virtual health, and that’s a great way to reach out to your provider to get directions to get tested without going to a doctor’s office. This is how OhioHealth is currently operating.
For those who do not have primary care physicians, it may be more challenging. I would say you need to figure out how to plug into telemedicine or to get health care for appropriate testing without being seen by a provider. We want to avoid people who have COVID-19 or flu-like symptoms going to a doctor’s office and exposing other people.
Can we plan for the flu season by observing what happens in the Southern Hemisphere? (14:29)
Most of the time what happens in the Southern Hemisphere matches what happens for us in the Northern Hemisphere. This year, the WHO has reported that influenza activity in the Southern Hemisphere is very mild to nonexistent. It’s my opinion that this has to do with mask-wearing. Everything we’re doing to protect against COVID-19 – hand hygiene, wearing a mask, social distancing, being outdoors instead of indoors – also applies to all respiratory viruses. I’m hopeful that we’ll follow in the footsteps of the Southern Hemisphere this flu season.
Could you explain more about masks, such as how they are beneficial, how to properly wear one and what type of mask is best? (15:35)
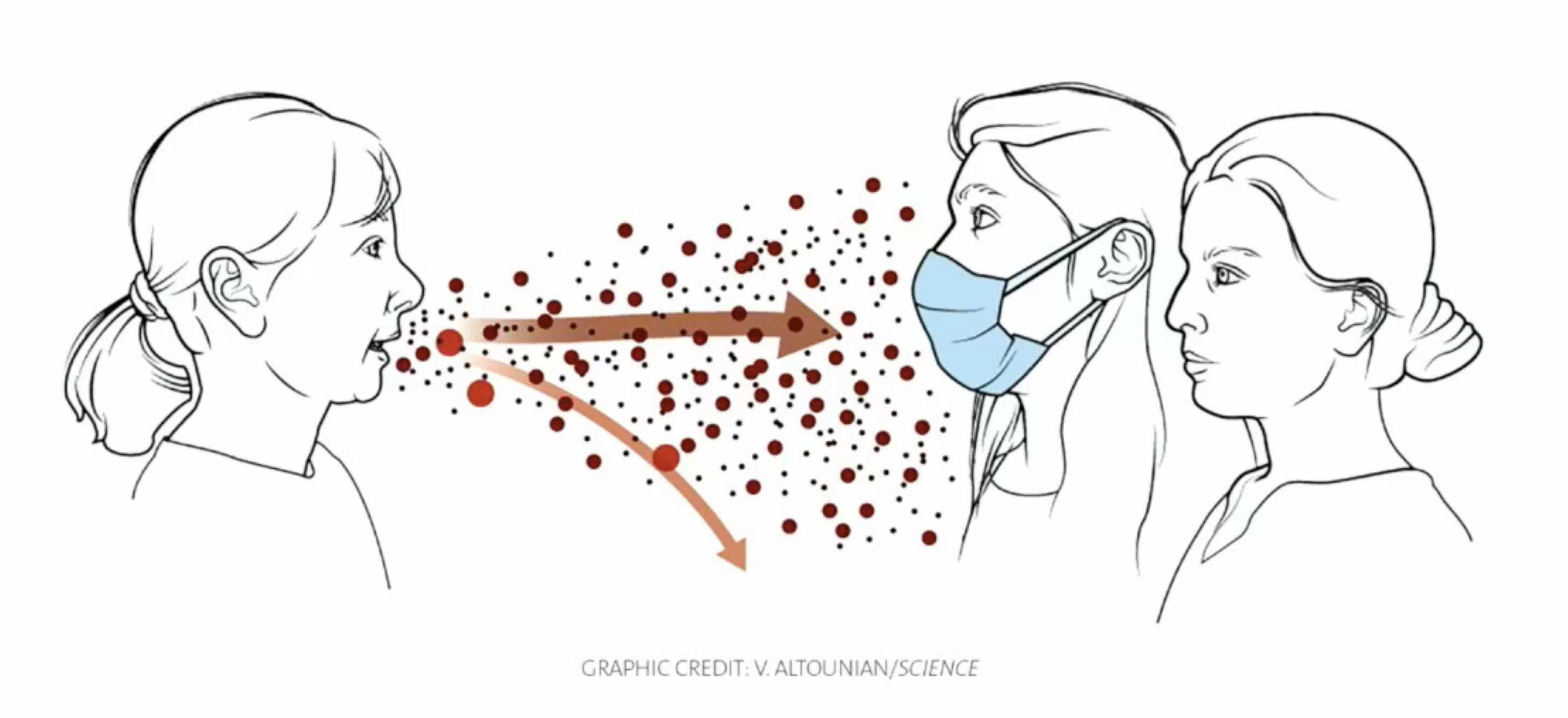
Wearing a mask offers protection in two ways.
The first is if I have COVID-19, flu or any other respiratory viruses, my droplets are less likely to spread. Whether I’m coughing, sneezing, or talking loudly, my mask is catching the infected droplets and keeping those around me safe.
The second thing that we now recognize is the mask does offer some protection to the wearer. So, if I’m wearing a mask, and someone near me has any respiratory viruses, their droplets would hit my mask first. Having a layer protecting my mucous membranes greatly decreases my chance of infection.
Therefore, it’s important to wear a mask but to also wear it properly. Face masks need to cover your nose, mouth and chin. Make sure you pinch the mask at the bridge of your nose, in order to create a good seal. Overall, you want to have a snug fit.
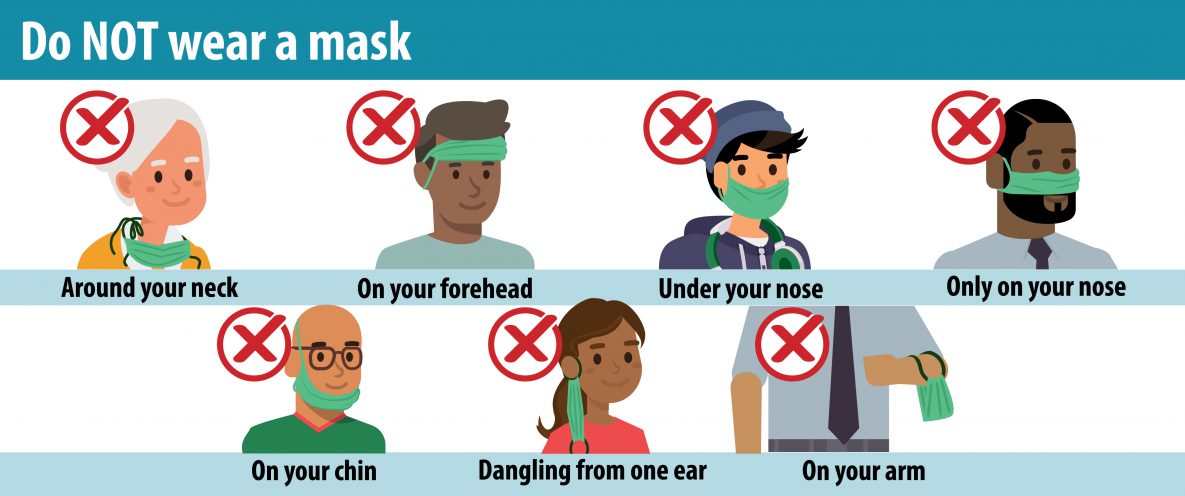
You don’t want to have your mask on in any of the ways shown above as these methods offer no protection at all. If you are eating or drinking, it’s okay to take your mask off as long as you are protecting it. The best way to do so is by storing your mask in something that breathes, such as a paper bag or envelope, when you are not using it.

A question I get a lot is, “What is the best type of mask to wear?” You want a mask that has a lot of layers, such as a mask with cotton in it. If you look at cotton under a microscope, you will see a bunch of organic fibers woven together. This provides a lot more protection than masks made of synthetic fibers, such as nylon, can. Nylon is the same material that pantyhose is made of. When you stretch out pantyhose, a lot of small holes appear, which allows air to go through them. Therefore, an organic, thick, double-layered cotton mask is the best type of mask to wear in public.
You should not wear a mask that you can’t breathe through, one made of vinyl or plastic, or one that has an exhalation valve. If you have a respiratory virus, a valve would allow the virus to leave the mask when you exhale. This endangers everyone around you, and only aids the spread of viruses.
Finally, N95 masks should not be worn in public. We want to save those for healthcare workers. I’m very happy to say our supply of personal protective equipment on the hospital side is good, but we don’t know what our supply needs are going to be come influenza season. Therefore, we should reserve medical supply personal protective equipment for healthcare use only.
Is it okay for me to remove my mask while outside, for example, at a sporting event? (21:00)
If you’re outside and your mask is removed, you really want to watch your social distancing. If you’re in a crowded area with a bunch of people outside, especially if they’re yelling or cheering on their team, that’s more of a venue for droplets to be transmitted. So yes, if you’re outside, you can remove your mask, but you have to be very sensitive to what’s going on around you. Bottom line: If you’re taking your mask off for a break, do it far away from where people are celebrating, yelling and rooting on their team.
My glasses fog up when I wear a mask. How can I mitigate this? (22:14)

You really want to get a mask that has a tight fit. This will prevent your breath from going up and steaming your glasses. Experiment with masks until you find a suitable one that has a good fit around the arch of the nose. Lately, I have been seeing a lot of people wearing a facial shield. I want to emphasize that facial shields are not a good substitute for a mask.

When it comes to kids, you want to make sure they have a pediatric or child mask, so it fits properly to their face. An adult mask will not fit properly and therefore will offer less protection. If you’re unsure of where to purchase one, I recommend looking at Old Navy and Dick’s Sporting Goods, as I have seen them sold there. Don’t worry about children younger than 2, as we don’t have appropriate masks to fit those ages.
Finally, it’s important to provide mask education to children so they can remove their mask, especially if they fall. Overall, if you can’t find a mask that fits properly, you want to do the best you can to make sure it covers the nose, mouth and chin.
What is something parents can tell their children to do when they go to school? (24:37)
The two most important mitigation strategies are to wear a mask and social distance because the predominant way COVID-19 and flu are spread is through droplets. Along with this, we still need to emphasize hand hygiene, not touching your eyes, nose and mouth, and to vocalize when you are not feeling well. We need to normalize not going to school or work when you’re not feeling well, for the safety of our communities. As an infectious disease doctor, I wish we would have had this cultural message for years. It’s safer for everyone.
How do I take off a mask properly? (26:29)
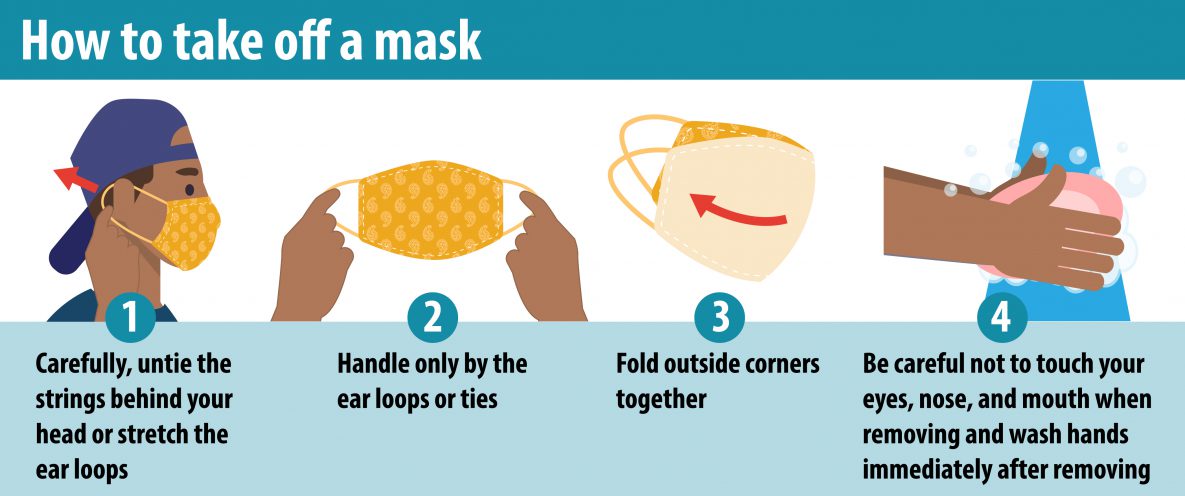
A mask is not sterile, so it’s important to know how to take it off properly.
When wearing a medical-grade mask, the blue outside of the mask is the part that you want to keep as clean as possible. Try not to touch this part, as it’s where the virus lands, and you can contaminate it or potentially yourself. If you want to manipulate your mask while you’re wearing it, only touch the edges.
When you take your mask off, you want to remove the loops around your ears. Fold the mask in half, protecting the outside part. You want the inside of your mask exposed. Once folded, store your mask so it has the opportunity to dry out. As mentioned earlier, this can be done by storing it in a paper bag or envelope. Once stored, go ahead and sanitize your hands. Now you’re done and your mask is safe.
When you want to put your mask back on, take it out of the bag and unfold it by only touching the loops and edges. Once on, make a seal at the bridge of your nose and pull the bottom down until it covers your nose, mouth and chin. Remember: one mask per day. Think of your mask like underwear – wear it once a day, then launder it (if it’s a reusable mask). At the start of the day when you put your mask on, you should inspect it to make sure it doesn’t have holes in it and that it’s not soiled.
Will the COVID-19 vaccine philosophy be similar to how the flu vaccine is encouraged? (29:28)
It’ll be encouraged. First of all, let’s talk about the flu vaccine. It’s been around for a long time, we’re very familiar with it, and it’s officially approved by the Federal Drug Administration for anybody 6 months or older. We’ve always emphasized that vulnerable people, such as those with health conditions or pregnant people, should get the flu vaccine. It’s important for pregnant people to receive the vaccination because it vaccinates both the individual and their baby, which is helpful since the flu vaccine is not given to those under 6 months of age.
There are many different vaccines being studied right now for COVID-19, and some are even in phase 3 of their trials. When we do have a vaccine that is available and is both FDA- and company-approved, we want people to understand the safety of the vaccine and to choose to get the vaccine. We would like to get a 60–70% herd immunity, which occurs when a large portion of a community becomes immune to a disease. This can happen through vaccination, and if enough people have recovered and developed antibodies.
This article is based off of a live interview conducted on Facebook on September 10, 2020. Due to the changing nature of COVID-19, some information might be dated. Always check the CDC’s website for the latest information concerning COVID-19.